
Medical Director &
Senior Consultant Surgeon
B Med Sci (Nottingham), MBBS (Nottingham), MMed (Surgery), FRCS (Edinburgh), FAMS

Senior Consultant
Colorectal Surgeon
MBBS (Singapore), MMed (Surgery), FRCS (Edinburgh), FAMS

Senior Consultant
Colorectal Surgeon
MBBS (Singapore), MMed (Surgery), FRCS (Edinburgh), FAMS
Hearing that colorectal cancer surgery may be recommended often raises many questions, especially when much of the information available comes from online sources or personal accounts. It is not uncommon for these sources to present mixed or outdated views, which can make it harder to understand what the procedure actually involves. Concerns about recovery, daily activities and possible long-term effects are valid, but they are sometimes influenced by misconceptions rather than current medical practice.
Today, colorectal surgery is guided by established clinical standards and continues to improve with advances in technique and care. While every individual's situation is different, many of the common beliefs about surgery do not fully reflect what most patients experience. Having clear, reliable information can help you better understand what to expect and support more informed discussions with your doctor.
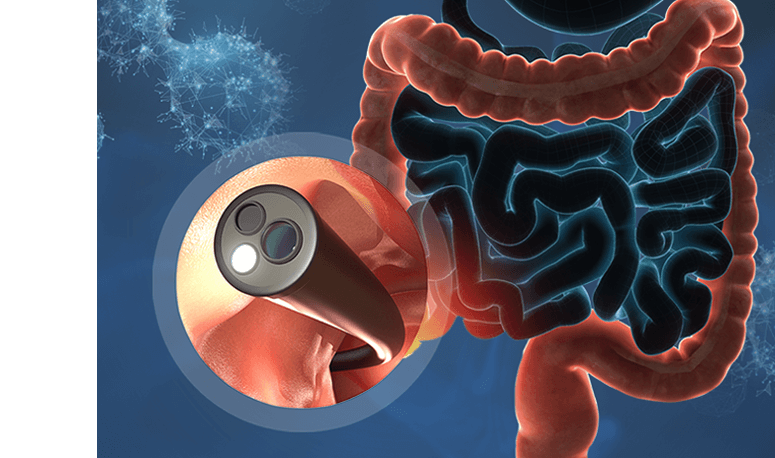
Understanding Colorectal Cancer Surgery
Colorectal cancer surgery is planned based on several factors, including where the tumour is located, how far it has developed and your overall health. Rather than a one-size-fits-all procedure, the operation is tailored to remove the cancer while maintaining bowel function as much as possible. This is why two people with the same diagnosis may still be recommended different surgical approaches.
One area that often causes confusion is how surgery affects daily life afterwards. Not all patients require a stoma, and when one is needed, it may be temporary depending on the situation. Recovery timelines, diet adjustments and activity levels can also vary, and are usually guided by your care team based on your progress. Understanding these variables helps explain why experiences differ, and why some commonly shared assumptions may not apply in every case.
Common Myths About Colorectal Cancer Surgery
Myth 1: Surgery always results in a permanent stoma
Not all colorectal cancer surgeries require a stoma. In cases where a stoma is needed, it may be temporary to allow healing before the bowel is reconnected. Whether a stoma is required depends on factors such as tumour location and surgical planning.
Myth 2: Recovery is always long and difficult
Recovery experiences can vary. Some patients may require more time, especially if the surgery is more complex, but others are able to return to their usual activities gradually with appropriate care and follow-up. Recovery plans are typically guided by the healthcare team.
Myth 3: Surgery means a permanent change in daily activities
While there may be adjustments during recovery, many people are able to resume their usual routines over time. Recommendations on diet and activity are usually tailored and may change as recovery progresses.
Myth 4: Minimally invasive surgery is not suitable for cancer
Minimally invasive techniques, such as laparoscopic surgery, may be considered for certain patients. The suitability depends on individual clinical factors, and your doctor will advise on the most appropriate approach.
Myth 5: Surgery alone is always enough to treat colorectal cancer
Surgery is an important part of treatment, but it may be combined with other therapies depending on the stage and characteristics of the cancer. Treatment plans are individualised based on clinical assessment.
What to Expect Before and After Colorectal Cancer Surgery
While individual experiences vary, there are general steps in the care process that most patients can expect, from pre-surgical assessments to recovery and follow-up.
Before Surgery
Before the procedure, you will typically undergo assessments such as imaging scans, blood tests and a review of your overall health. These help guide surgical planning and reduce risks. Your doctor will also explain the procedure, possible outcomes and any preparation required, which may include dietary adjustments or bowel preparation.
After Surgery
After surgery, you can expect a period of monitoring in the hospital, followed by gradual recovery at home. The length of stay and recovery timeline vary depending on the type of surgery and individual factors. Your care team will provide guidance on wound care, activity levels and follow-up appointments.
Recovery and Follow-up
Recovery does not end after discharge. Follow-up visits are important to monitor healing and overall progress. Some patients may require additional treatment, depending on their condition. Guidance on diet, physical activity and returning to daily routines is usually adjusted over time based on how you recover.
Making Sense of Your Colorectal Cancer Surgery Journey
Concerns about colorectal cancer surgery are often shaped by a mix of information, assumptions and personal accounts, which can make it difficult to form a clear and accurate understanding. In reality, surgery is not a one-size-fits-all experience but one guided by individual clinical factors, careful planning and established standards of care. Recognising this helps place common misconceptions in context and allows for more grounded, informed discussions about what to expect and what may be appropriate for your situation.
At our colorectal cancer surgery clinic, care is provided by Dr Dennis Koh, Dr Sharon Koh and Dr Pauleon Tan, who work together to assess each patient's condition and recommend appropriate, evidence-based treatment options. If you have concerns or questions about colorectal cancer surgery, consider scheduling an appointment with us to better understand your options and next steps.
Our Colorectal Surgeons

Dr Dennis Koh
Medical Director & Senior Consultant Surgeon
B Med Sci (Nottingham), MBBS (Nottingham)
MMed (Surgery), FRCS (Edinburgh), FAMS
Dr Dennis Koh is a MOH-accredited and experienced colorectal surgeon with specialised expertise in the management and treatment of colorectal cancer; and currently the Medical Director at Colorectal Practice.
Dr Koh strives to provide a customized treatment plan for each patient, which allows for better outcomes. He also honed his skills in proctology abRd in Geneva, bringing a more diverse touch to his practice.

Dr Sharon Koh Zhiling
Senior Consultant Surgeon
MBBS (Singapore), MMed (Surgery),
FRCS (Edinburgh), FAMS
Dr Sharon Koh is an experienced colorectal surgeon and the former Director of Endoscopy at Alexandra Health. She has subspecialty training in colorectal surgery, minimally invasive surgery, and advanced endoscopy — particularly in the field of colorectal cancer.
Dr Koh completed her fellowship at Cedars-Sinai Medical Centre in the US after being awarded the Academic Medicine Development Award by the National University Hospital.

Dr Pauleon Tan Enjiu
Senior Consultant Surgeon
MBBS (Singapore), MMed (Surgery),
FRCS (Edinburgh), FACS
Dr Pauleon Tan has served in public hospitals for over 15 years and is experienced in minimally invasive surgery and endoscopy. He is also experienced in the treatment for colorectal cancer, and strives to provide the best possible care to his patients.
Dr Tan undertook advanced colorectal surgical training at Japan’s Saitama International Medical Center after being awarded the Ministry of Health – Health Manpower Development Plan (HMDP) Award.