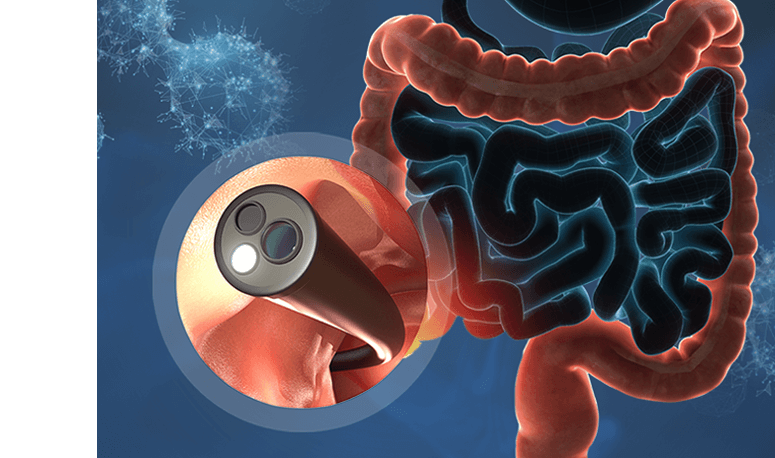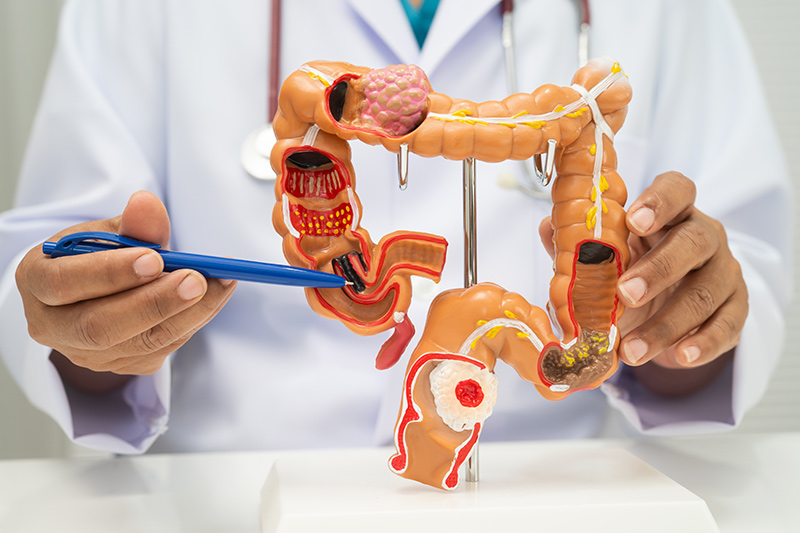
A colon polypectomy is the clinical removal of polyps—clumps of cells forming on the lining of the large intestine—during an endoscopic examination. While often asymptomatic, these growths are the primary precursors to colorectal malignancies, making their early extraction essential. By performing a colon polyp removal, specialists can effectively interrupt the progression of precancerous cells and reduce the long-term necessity for colon cancer surgery.
What Is a Colon Polypectomy?
A colon polypectomy is a minimally invasive surgical procedure that excises polyps directly from the lining of the large intestine (colon) or rectum. Performed during a colonoscopy, this technique allows a specialist to remove abnormal growths without the need for traditional open surgery or external incisions.
Colon polypectomies are both diagnostic and therapeutic, utilising high-definition imaging and specialised instruments to ensure the bowel is cleared of potentially hazardous lesions.
The process involves several precise clinical steps to ensure the safe and complete removal of the tissue:
- Endoscopic Access — A thin, flexible tube called a colonoscope is navigated through the bowel, providing a real-time, magnified view of the intestinal wall to locate even the smallest growths.
- Mechanical Extraction — Once a polyp is identified, surgical tools—such as wire loops (snares) or forceps—are passed through a channel in the scope to perform the polyp removal immediately.
- Thermal Ablation (Electrocautery) — In many cases, an electrical current is applied to the base of the polyp to burn through the tissue, which simultaneously seals blood vessels to prevent bleeding.
- Histological Analysis — Every excised specimen is preserved and sent to a laboratory for microscopic examination. This determines if the cells were benign, precancerous, or malignant.
Who May Require a Colon Polypectomy?
While anyone can develop intestinal growths, the following groups are most frequently advised to undergo colon polyps treatment to mitigate future health risks:
- Individuals Aged 45 and Above — As the risk of developing abnormal growths increases with age, routine screening is recommended for this demographic to detect and remove polyps early.
- Patients with Symptomatic Polyps — Those experiencing unexplained rectal bleeding, persistent abdominal pain, or significant changes in bowel habits often require an investigation and potentially colon polyp removal.
- Individuals with a Personal or Family History — A history of colorectal polyps or a family lineage of colon cancer necessitates more frequent surveillance and proactive intervention.
- Patients with Genetic Predispositions — Those diagnosed with hereditary conditions such as Lynch syndrome or familial adenomatous polyposis (FAP) require regular polypectomies to manage high-speed polyp formation.
- Individuals with Inflammatory Bowel Disease (IBD) — Chronic inflammation from conditions like ulcerative colitis can lead to dysplastic growths that require clinical extraction to prevent malignant transformation.
Early intervention is the most effective way to manage colorectal health and prevent the progression of asymptomatic growths.
If you meet any of the clinical criteria above, schedule a screening to ensure proactive detection and treatment.
Preparation Before Colon Polyp Removal
To ensure a safe and successful colon polyp removal, the following preparation steps are essential:
- Strict Bowel Preparation (Purging) — Patients must consume a prescribed clinical laxative solution the day before the procedure to thoroughly cleanse the colon of all faecal matter.
- Clear Liquid Diet — A 24-hour dietary restriction is required, limited to clear liquids such as broth, black coffee, and water to prevent new waste from forming.
- Medication Disclosure — It's critical to inform your specialist of all regular medications, particularly blood thinners like aspirin or warfarin, which may need to be paused to reduce bleeding risks.
- Fasting (NPO) — Patients are required to stop all oral intake, including water, for a specific number of hours before the procedure to ensure the sedation can be administered safely.
- Arranging Transportation — Because the procedure involves sedation, patients must arrange for a responsible adult to accompany them home, as driving is strictly prohibited for 24 hours.
How Is a Colon Polypectomy Performed?
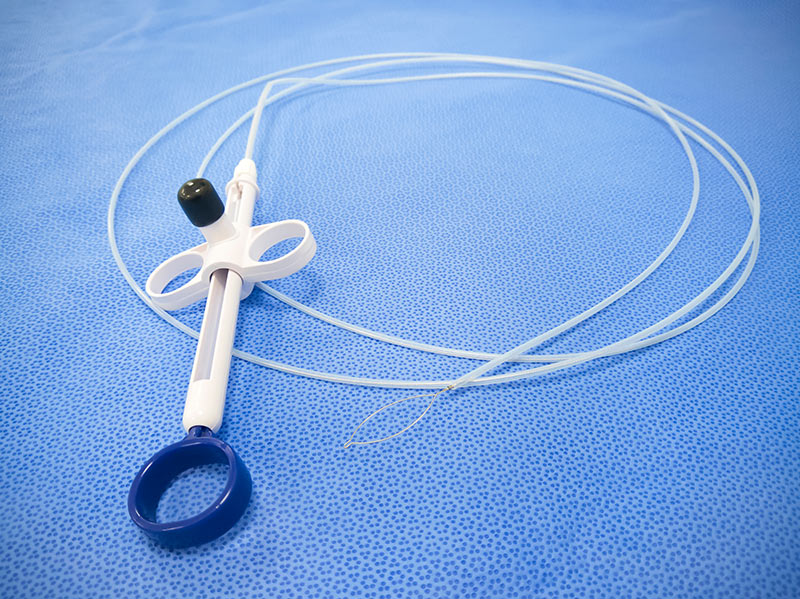
The procedure begins with the insertion of a colonoscope, providing a clear view of the intestinal lumen. Once a growth is identified, the scope remains in position to serve as a stable conduit for the specialised instruments required for removal.
Clinical Removal Techniques
The choice of method depends on the morphology, size, and location of the growth. Various techniques are employed to ensure the tissue is removed cleanly while minimising the risk of bleeding or perforation:
- Biopsy Forceps — Small instruments are passed through the scope to snip off diminutive polyps or take tissue samples. This is often the preferred method for growths only a few millimetres in size, ensuring a quick and efficient extraction.
- Cold Snare Polypectomy — Primarily used for small polyps under 5mm, a thin wire loop is placed around the base of the growth and tightened to mechanically cut the tissue. This technique avoids heat, reducing the risk of delayed complications.
- Hot Snare Polypectomy — For larger or pedunculated polyps, an electrical current passes through the wire snare as it closes. This thermal energy cauterises the site immediately, which is essential for sealing blood vessels and preventing haemorrhage.
- Endoscopic Mucosal Resection (EMR) — This advanced technique is reserved for large or flat sessile lesions. A saline solution is injected beneath the polyp to lift it away from deeper muscle layers, allowing for a deeper removal without damaging the bowel wall.
Accurate polyp removal requires a high degree of clinical precision and the selection of the appropriate surgical technique for each unique lesion.
Consult our specialists to ensure your procedure is performed using the latest minimally invasive methods for optimal safety and recovery.
What to Expect After a Colon Polypectomy
After the removal of polyps, the focus shifts to ensuring the mucosal lining heals correctly and monitoring for any rare complications. Following these clinical guidelines helps ensure a smooth recovery and provides clarity on the next steps of your diagnostic journey:
- Recovery and Observation — Following the procedure, you will remain in a recovery ward for approximately 30 to 60 minutes as the effects of the sedation subside. Clinical staff will monitor your vital signs and ensure you are comfortable before you are discharged to the care of a family member or friend.
- Possible Post-Procedure Symptoms — It's common to experience mild abdominal bloating or gas as the air used to expand the colon during the procedure escapes. You may also notice a very small amount of blood during your first bowel movement, which is typically a normal result of the tissue excision and should resolve quickly.
- Follow-Ups After Colon Polyps Removal — All extracted polyps are sent to a laboratory for histological analysis to determine their exact cellular makeup. Your specialist will schedule a follow-up consultation, usually within one to two weeks, to discuss these results and establish a personalised schedule for your next surveillance colonoscopy.
- Risks and Complications of Colon Polypectomy — While this is a safe and routine procedure, potential risks include delayed bleeding at the excision site or, very rarely, a small tear in the colon wall (perforation). If you experience severe abdominal pain, a firm or tender abdomen, or a significant fever in the days following the procedure, you should seek immediate medical assessment.
Take Proactive Steps Toward Digestive Wellness
Early detection through regular screenings is a critical step in preventing advanced disease and maintaining long-term bowel health. If you have concerns about your digestive health or are due for a routine check-up, consulting our experienced colorectal surgeons—Dr Dennis Koh, Dr Sharon Koh and Dr Pauleon Tan—can provide the expert assessment and personalised care needed to ensure the best possible outcomes.
To discuss your symptoms, learn more about Colorectal Practice's specialised diagnostic services, or schedule a screening appointment, please contact us today.
Frequently Asked Questions About Colon Polypectomy
Is colon polyp removal painful?


How long does a colon polypectomy take?


Can colon polyps grow back after removal?


How soon can normal activities be resumed?


Is colon polypectomy considered surgery?


Our Colorectal Surgeons

Dr Dennis Koh
Medical Director & Senior Consultant Surgeon
B Med Sci (Nottingham), MBBS (Nottingham)
MMed (Surgery), FRCS (Edinburgh), FAMS
Dr Dennis Koh is a MOH-accredited and experienced colorectal surgeon with specialised expertise in the management and treatment of colorectal cancer; and currently the Medical Director at Colorectal Practice.
Dr Koh strives to provide a customized treatment plan for each patient, which allows for better outcomes. He also honed his skills in proctology abRd in Geneva, bringing a more diverse touch to his practice.

Dr Sharon Koh Zhiling
Senior Consultant Surgeon
MBBS (Singapore), MMed (Surgery),
FRCS (Edinburgh), FAMS
Dr Sharon Koh is an experienced colorectal surgeon and the former Director of Endoscopy at Alexandra Health. She has subspecialty training in colorectal surgery, minimally invasive surgery, and advanced endoscopy — particularly in the field of colorectal cancer.
Dr Koh completed her fellowship at Cedars-Sinai Medical Centre in the US after being awarded the Academic Medicine Development Award by the National University Hospital.

Dr Pauleon Tan Enjiu
Senior Consultant Surgeon
MBBS (Singapore), MMed (Surgery),
FRCS (Edinburgh), FACS
Dr Pauleon Tan has served in public hospitals for over 15 years and is experienced in minimally invasive surgery and endoscopy. He is also experienced in the treatment for colorectal cancer, and strives to provide the best possible care to his patients.
Dr Tan undertook advanced colorectal surgical training at Japan’s Saitama International Medical Center after being awarded the Ministry of Health – Health Manpower Development Plan (HMDP) Award.