
Dr Dennis Koh
Medical Director & Senior Consultant Surgeon
B Med Sci (Nottingham), MBBS (Nottingham), MMed (Surgery), FRCS (Edinburgh), FAMS
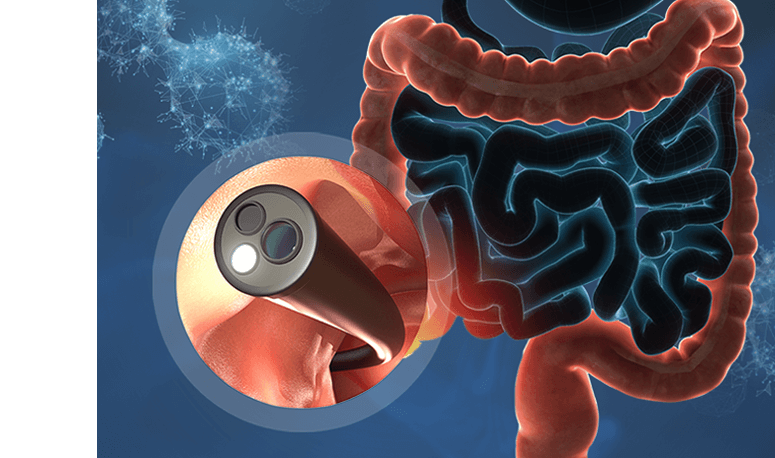
Recovery after colorectal surgery is a gradual and structured journey that continues well beyond hospital discharge. Whether the procedure was performed for colorectal cancer, diverticular disease, inflammatory bowel conditions or other bowel disorders, the weeks and months that follow are just as important as the surgery itself. Steady progress, careful monitoring and consistent self-care all play a key role in achieving a stable, long-term outcome.
Immediate Post-surgery Recovery (Hospital Stay)
The immediate recovery phase begins in the recovery ward and continues throughout your hospital stay. This period typically ranges from 3 to 7 days, depending on the specific surgical technique used and your individual rate of progress.
Physical Recovery
During the initial 24 to 72 hours, the primary clinical focus is on physical stabilisation. Patients typically navigate the following recovery milestones:
- Management of Surgical Discomfort: Localised abdominal pain or soreness around the incision sites is expected. This is carefully managed using oral medications or patient-controlled analgesia to ensure you remain comfortable as you heal.
- Anaesthesia-related Fatigue: It's common to experience significant fatigue, drowsiness, or a lack of appetite as the effects of anaesthesia subside. These symptoms are temporary and gradually resolve as your body stabilises.
- Resumption of Bowel Activity: A temporary pause in bowel function often occurs immediately after surgery. To encourage activity, patients are assisted in sitting up and walking short distances as early as possible.
- Promotion of Early Mobilisation: Moving shortly after surgery is vital for a smooth recovery. Early physical activity supports digestive function and significantly reduces the risk of post-operative blood clots.
Bowel Function
The resumption of digestive activity is a primary clinical milestone required for hospital discharge. You may notice several signs that your system is successfully recovering:
- Evidence of Internal Activity: Hearing bowel sounds or passing gas are positive indicators that the digestive tract is beginning to function again.
- Initial Bowel Movements: Successfully having your first bowel movement confirms that the system is operational, even if the consistency is not yet normal.
- Management of Early Irregularity: It's common to experience bloating, diarrhoea, or delayed stools during this early phase. These fluctuations are a standard part of the healing process and usually do not signify a complication.
Diet Progression
After surgery, your digestive system requires time to recover. Most patients begin with clear fluids before gradually progressing to soft or low-fibre foods as tolerated. Heavy, greasy or spicy foods should be avoided during the early phase, as they may cause discomfort or bowel irritation.
A reduced appetite is common in the first few days after surgery. There is no need to force large meals. Instead, take small, balanced portions and maintain adequate hydration while your appetite gradually returns.
Early Recovery Phase (First 2 to 4 Weeks)
This phase begins after discharge and is where most complications occur if recovery is poorly managed.
Activity and Mobility
Frequent movement is essential for a smooth recovery, though it must be balanced with targeted rest. Prioritising gentle activity while respecting physical limits helps ensure a steady return to strength.
- The Importance of Daily Walking: Walking several times a day is encouraged, even if you feel mild discomfort. Regular movement supports healthy circulation, stimulates bowel function, and accelerates the overall healing process.
- Adhering to Physical Restrictions: To protect the surgical site, avoid lifting heavy objects, driving long distances, or engaging in strenuous exercise. Specifically, refrain from any activities that strain the abdominal muscles during the initial weeks.
- Managing Post-operative Fatigue: Feeling physically weak or easily exhausted is a normal response to surgery, even if you appear outwardly well. Prioritise adequate rest and allow your body the time it needs to recover its natural energy levels.
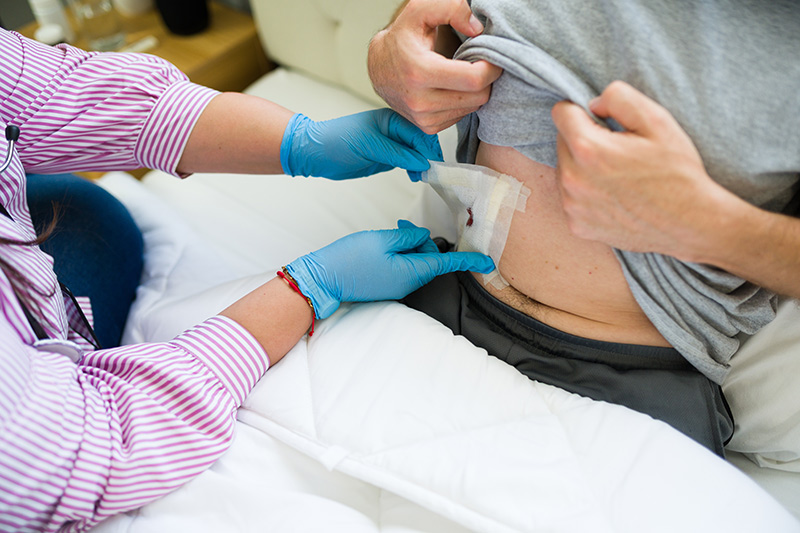
Wound Care
Careful wound care is important after colorectal cancer surgery. Keep the surgical site clean and dry, and follow your doctor's instructions for dressing changes. Avoid applying any creams or remedies unless prescribed. You should also seek medical attention promptly if you notice increasing redness, swelling, discharge, fever or worsening pain, as these may be signs of infection that require early treatment.
Bowel Changes
It's normal to experience loose stools, urgency, constipation, gas or bloating during the early recovery phase. These symptoms are usually temporary and improve over time. However, seek medical attention promptly if you're unable to pass stools or gas, develop severe abdominal distension or notice worsening abdominal pain, as these may require urgent review.
Intermediate Recovery Phase (1 to 3 Months)
During this stage, many patients begin returning to more regular routines. However, recovery is still ongoing, and caution remains important.
Return to Work
Patients with office-based roles may return to work after 4 to 6 weeks, provided their energy levels and symptoms have stabilised. Conversely, roles involving manual labour, heavy lifting, or prolonged standing typically require a more extended recovery period to ensure physical safety.
Returning too early can lead to persistent fatigue, increased abdominal discomfort, or delayed wound healing. It also elevates the risk of developing an incisional hernia; therefore, a gradual return guided by your specialist is essential for a secure long-term recovery.
Physical Conditioning
You may begin gentle strengthening exercises and light stretching once your surgeon provides clinical approval. However, high-impact sports, heavy weightlifting, and intensive gym training must still be avoided during this critical phase.
Although the surface incision may appear fully healed, the deeper abdominal and core muscles require more time to recover internally. Prioritising the protection of these deep tissues is essential to reduce the risk of internal strain and long-term surgical complications.
Diet Normalisation
Patients can gradually reintroduce fibre-rich foods—including vegetables, fruits, and whole grains—as their digestive tolerance improves. It's important to increase fibre intake slowly to prevent unnecessary bloating or abdominal discomfort during the transition.
Maintaining adequate hydration is also essential throughout this phase. Dehydration can exacerbate bowel symptoms such as constipation or cramping, a risk that is particularly heightened in Singapore's warm and humid climate.
Ongoing Bowel Adjustment
Some patients may experience long-term changes in bowel habits following surgery. While these shifts can be initially concerning, most individuals adapt well through clinical guidance and simple lifestyle adjustments; in some instances, medication may also be used to manage symptoms effectively.
Common changes include increased stool frequency, reduced urgency control, or new sensitivities to specific foods. Through structured follow-up care and tailored dietary advice, most patients successfully regain their confidence and maintain an excellent quality of life.
Long-term Recovery and Lifestyle Adjustments

Long-term recovery extends beyond physical healing, focusing on the sustained maintenance of bowel health and the proactive prevention of disease recurrence.
Follow-up Care
Regular follow-up appointments are a vital component of your long-term recovery and clinical monitoring. Skipping these scheduled reviews may delay the detection of potential complications or early signs of disease recurrence.
During these visits, your specialist may perform physical examinations or request blood tests, colonoscopies, and imaging studies when clinically indicated. These proactive assessments help monitor your internal healing and ensure early intervention if any health concerns arise.
Diet and Weight Management
Maintaining a balanced diet is fundamental to supporting long-term bowel health and ensuring a smooth recovery. Gradual, healthy weight management is equally vital, as excessive weight gain can place undue pressure on abdominal tissues, increasing the risk of hernias and bowel dysfunction.
Smoking and Alcohol
Smoking significantly impairs tissue healing and elevates the risk of post-surgical complications. Similarly, alcohol can irritate the bowel and lead to dehydration, which may exacerbate recovery symptoms. It's best to avoid both during the healing period and limit their intake long-term to support your overall health.
Potential Complications to Watch For
While some discomfort and bowel changes are expected, certain symptoms are not part of normal healing and must never be ignored. If any of these concerning signs appear, early review by a medical professional is essential:
- Signs of Infection: Infection can occur at the surgical wound or internally, often presenting as fever, spreading redness, or foul-smelling discharge. Seek immediate care if you notice increasing pain or pus around the incision site.
- Blood Clots: Reduced mobility after surgery can lead to clots in the legs or lungs. Warning signs include sudden calf swelling, chest pain, shortness of breath, or coughing up blood.
- Bowel Obstruction or Severe Constipation: Obstructions from scar tissue or swelling can prevent the passage of stool or gas. Urgent attention is needed for severe bloating, persistent vomiting, or an inability to pass gas for several days.
- Emergency Symptoms: Sudden clinical changes such as black or bloody stools, fainting, a rapid heart rate, or severe pain that resists medication require immediate evaluation to rule out serious internal conditions.
Get Support From Our Colorectal Specialist
Navigating the recovery timeline after colorectal surgery requires a proactive approach to both physical healing and long-term lifestyle adjustments. While gradual progress is expected, any persistent irregularities or concerning symptoms should be evaluated by a specialist to ensure your recovery milestones are being met safely.
At Colorectal Practice, our Medical Director, Dr Dennis Koh, provides expert clinical oversight for patients transitioning from hospital care to long-term wellness. With a focus on minimally invasive techniques and personalised recovery plans, he and his team provide comprehensive support across four major medical centres in Singapore.
If you have questions regarding your post-operative progress or require a professional assessment of your recovery path, please message us at 6262 1226 or book an appointment via our website today.
Our Colorectal Surgeons

Dr Dennis Koh
Medical Director & Senior Consultant Surgeon
B Med Sci (Nottingham), MBBS (Nottingham)
MMed (Surgery), FRCS (Edinburgh), FAMS
Dr Dennis Koh is a MOH-accredited and experienced colorectal surgeon with specialised expertise in the management and treatment of colorectal cancer; and currently the Medical Director at Colorectal Practice.
Dr Koh strives to provide a customized treatment plan for each patient, which allows for better outcomes. He also honed his skills in proctology abRd in Geneva, bringing a more diverse touch to his practice.

Dr Sharon Koh Zhiling
Senior Consultant Surgeon
MBBS (Singapore), MMed (Surgery),
FRCS (Edinburgh), FAMS
Dr Sharon Koh is an experienced colorectal surgeon and the former Director of Endoscopy at Alexandra Health. She has subspecialty training in colorectal surgery, minimally invasive surgery, and advanced endoscopy — particularly in the field of colorectal cancer.
Dr Koh completed her fellowship at Cedars-Sinai Medical Centre in the US after being awarded the Academic Medicine Development Award by the National University Hospital.

Dr Pauleon Tan Enjiu
Senior Consultant Surgeon
MBBS (Singapore), MMed (Surgery),
FRCS (Edinburgh), FACS
Dr Pauleon Tan has served in public hospitals for over 15 years and is experienced in minimally invasive surgery and endoscopy. He is also experienced in the treatment for colorectal cancer, and strives to provide the best possible care to his patients.
Dr Tan undertook advanced colorectal surgical training at Japan’s Saitama International Medical Center after being awarded the Ministry of Health – Health Manpower Development Plan (HMDP) Award.